
Specialist in Internal Medicine & Geriatrics
Oon Chiew Seng Professor in Medicine, Healthy Ageing and Dementia Research
NUS Academy for Healthy Longevity
Yong Loo Lin School of Medicine,
National University of Singapore
The World Health Organization (WHO) defines healthy ageing as the process of developing and maintaining the functional ability that enables wellbeing in older age1. In reality, ageing is associated with the decreased ability to efficiently absorb certain micronutrients, which leads to changes in some nutritional requirements2. Of note, nutritional inadequacy conditions are silent epidemics affecting not only older adults but people of all genders and ages3. Accordingly, ensuring sufficient nutrient intake is crucial for reducing the risk of nutrient inadequacy-related health problems. Although foods fortified with micronutrients are available, the intake of certain nutrients was reported to be inadequate among older people4. In this regard, oral multivitamin and mineral (MVM) supplementation would provide a convenient solution to improve the nutritional status of this population.
Frailty is a condition in which multiple physiological systems decline in function due to loss of homeostasis. Multi-dimensional factors such as physical, psychosocial, and cognitive ability play a part in its development. Frailty has been reported to be associated with adverse outcomes such as mortality, fractures, and falls. Therefore, frailty must be prevented to ensure a healthy life expectancy without disease, particularly among older adults at an increased risk of frailty5.
Dietary quality is essential for promoting health and lowering the risk of diet-related frailty. In particular, various vitamins and minerals, such as vitamin A, B complex, D, calcium, iron, zinc, etc., are required for maintaining physiological functions. Thus, the deficit in one or more micronutrients would hinder normal physiological functions, resulting in adverse health outcomes. A recent review by Kiani et al. (2022) reported that micronutrient deficiency would lead to intellectual impairment, poor growth, perinatal complications, degenerative diseases associated with ageing and higher morbidity and mortality6. While older adults are more susceptible to adverse outcomes, preventing micronutrient inadequacy among this population is of paramount importance.
Of note, nutritional deficiency is a severe disease condition in which the levels of nutrients are significantly reduced, leading to complications and mortality6, whereas nutrient inadequacy is the suboptimal levels of nutrients that increase the risk of health problems.
Although a consensus on the clinical definition of micronutrient inadequacy is yet to be available, the abnormalities in micronutrient levels can be identified by blood tests. Additionally, patients with inadequate micronutrients could be differentiated based on symptoms. Examples of major symptoms of deficiency in selected micronutrients are listed in Table 16.
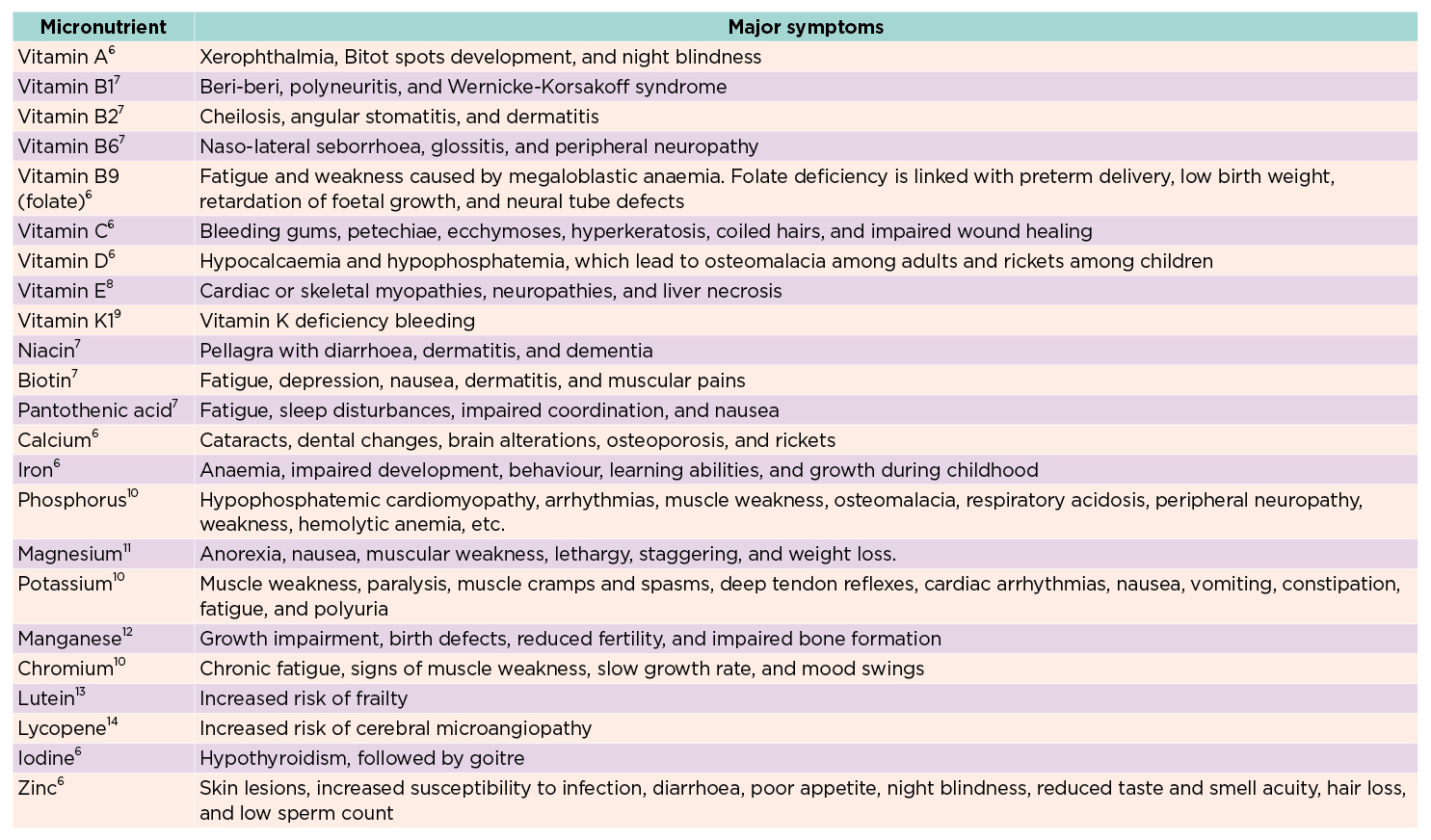
Table 1. Examples of micronutrients deficiency conditions
In view of the potential adverse outcomes, preventing micronutrient inadequacy is crucial. Fortunately, this can be readily achieved through supplementation and food-based approaches.
It is important to realise that the risk of micronutrient inadequacy is not limited in older adults. However, age and intake are the main contributing factors, given that micronutrient intake by older adults is generally not adequate. Remarkably, the amount of total food intake does not necessarily reflect the micronutrient intake since the micronutrient contents are variable in different kinds of food and can be changed upon food processing. Accordingly, a cross-sectional study by Houshialsadat et al. (2023) reported a negative association between quintiles of energy contribution of ultra-processed foods and dietary diversity (β=− 0.43, p<0.001). The overall micronutrient content was lower in the diet fraction dominated by ultra-processed foods than non-ultra-processed food diet fraction15. Thus, while the vitamin, mineral, and dietary fibre contents in highly processed food are very low, the older individuals who often consume them are unlikely to intake adequate micronutrients. This partially explains why micronutrient inadequacy is still possible despite the right amount of food intake.
The meta-analysis by Borg et al. (2015), which included 37 clinical studies accounting for >28,000 community-dwelling older adults aged ≥65 years in 20 different Western countries, indicated that the percentage of the population at risk for inadequate intakes of thiamine, riboflavin and vitamin D from food alone was >30% for both men and women. Regarding mineral intake, ≥30% of the population was at risk for inadequate intakes of calcium, magnesium and selenium from food alone (Figure 1A and 1B)16. The results highlighted the high prevalence of inadequacies in micronutrient intake among the older population.
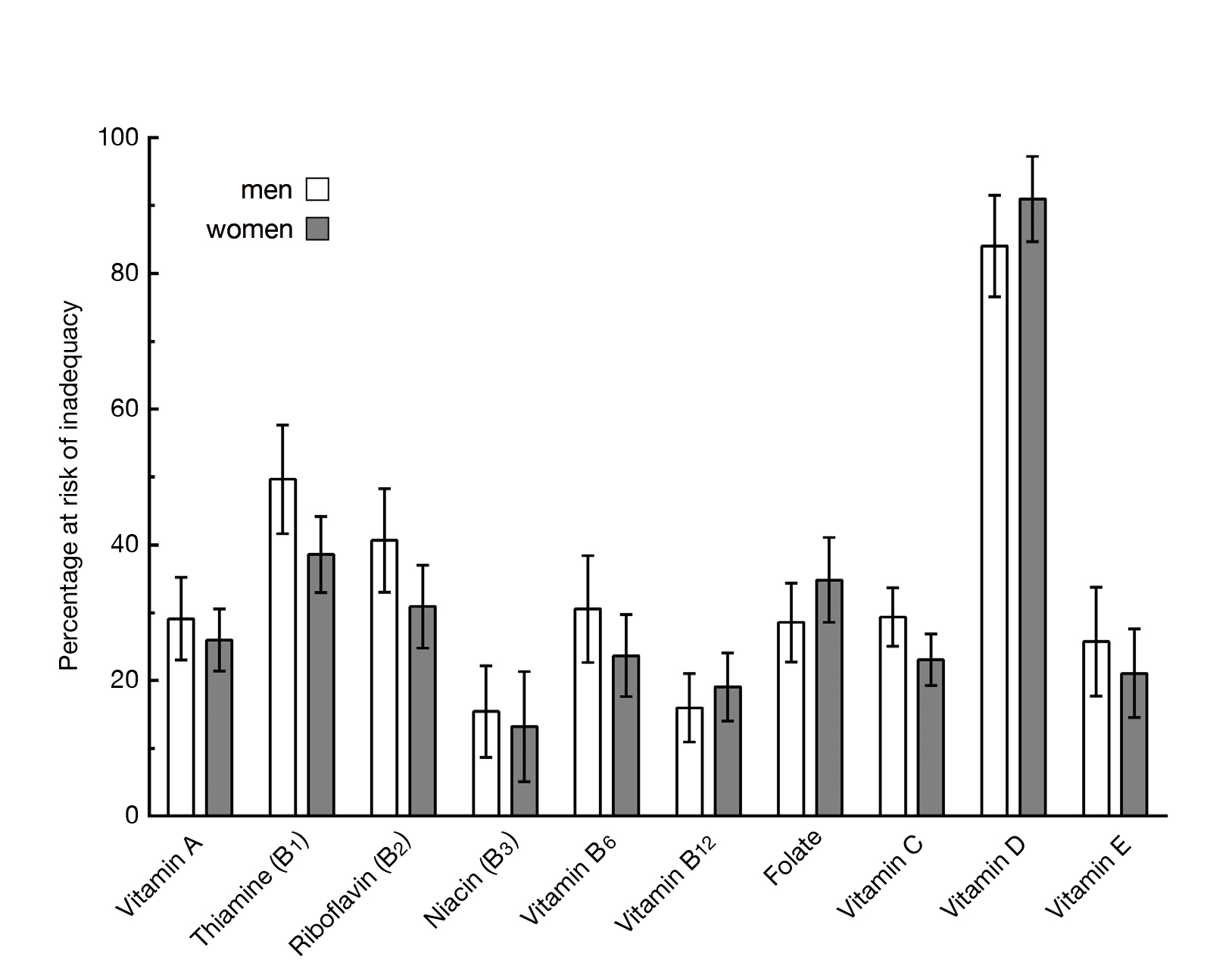
Figure 1A. Mean percentage of men and women aged ≥65 years at risk for inadequate intake of vitamins16
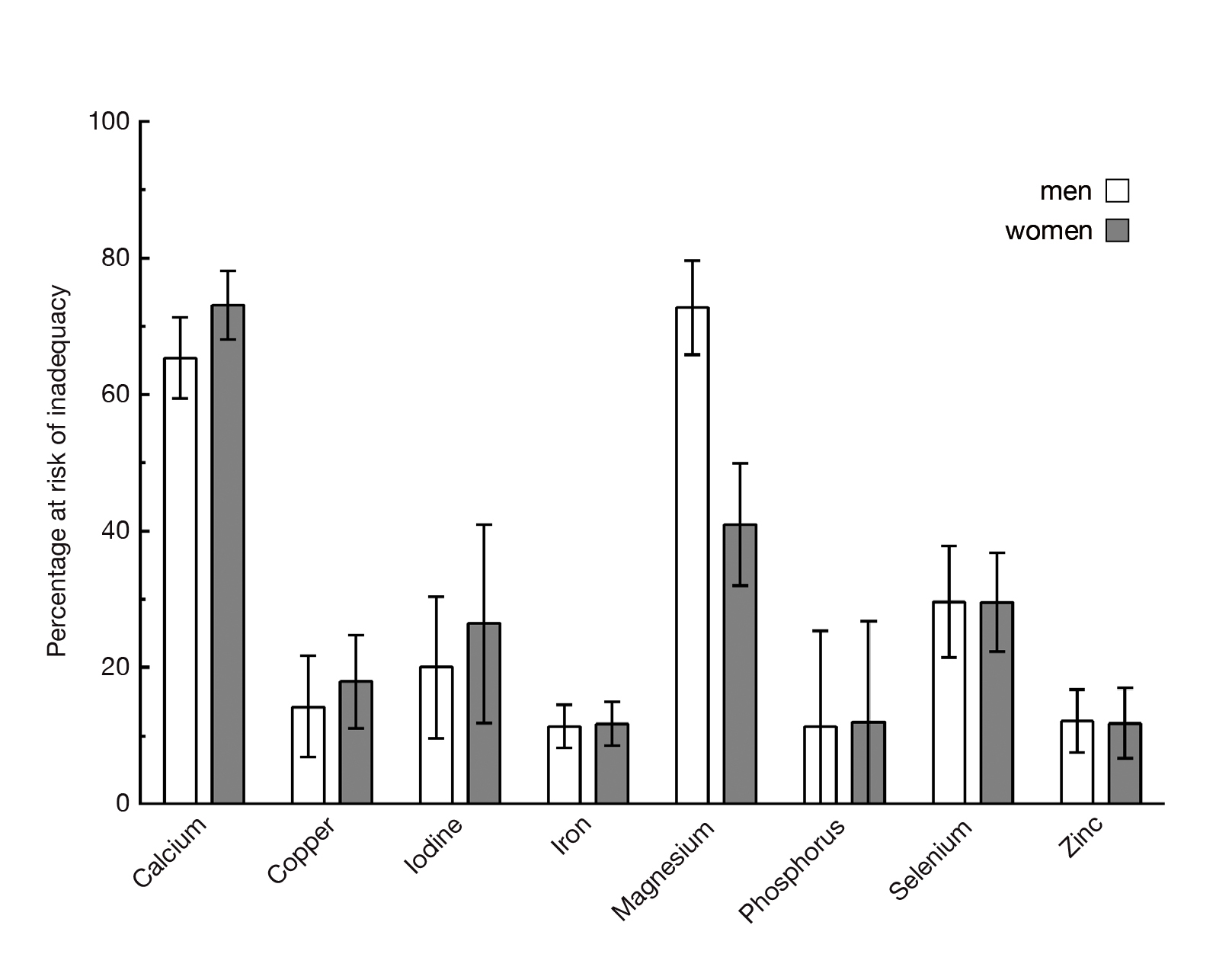
Figure 1B. Mean percentage of men and women aged ≥65 years at risk for inadequate intake of minerals16
In the scenario of Hong Kong, the Total Diet Study (2014) conducted by the Centre for Food Safety of the Food and Environmental Hygiene Department (FEHD) reported that >90% of Hong Kong adults had dietary calcium intake less than recommended level, and >80% had insufficient iron intake. Dietary intake of copper, magnesium, manganese, molybdenum and phosphorus were also inadequate as per recommended intakes17.
Apart from food intake, the changes in body composition of older adults also contribute to micronutrient inadequacy. Notably, the reduced lean body mass and increased fat stores result in reduced metabolic rate and energy requirements, respectively18. Importantly, the changes to the gastrointestinal (GI) tract on the utilisation of nutrient intake also affect the nutritional status among older adults. While suboptimal oral health is common among older adults, this would reduce appetite and, hence, food intake. On the other hand, the reduced GI motility and volume of digestive juices would lower the efficiencies of food digestion and absorption. Remarkably, the occurrence of age-related comorbidities, such as dementia and sarcopenia, would decrease the ability to self-care, increase frailty and morbidity, limit access to food19. This would potentially result in a vicious cycle of ill-health.
Interestingly, age-related changes in the gut microbiota also play a role in the development of micronutrient inadequacy. The gut microbiota of older adults is characterised by a reduced bacterial diversity, shifts in the dominant species, a decline in beneficial microorganisms, an increase in facultative anaerobic bacteria, and a decrease in the availability of total short-chain fatty acids (SCFAs)20. Particularly, Jackson et al. (2016) reported that there was a negative association between frailty and gut microbiota diversity21.
Thus, the optimisation of the overall nutritional status for older adults has to consider the factors in different aspects, including the amount and types of food consumed, the individual’s physiological conditions, and their lifestyle factors.
Nutrition needs vary by age, sex, physiological state, and lifestyle of the individuals. For instance, athletes need more protein, vitamin D, and adequate zinc than people who are not too active. In addition to behavioural factors, Jophlin et al. (2024) illustrated that patients with alcohol use disorder (AUD) may have nutritional deficiencies, especially isolated nutrient deficiencies, such as thiamine or zinc deficiencies22. By virtue of the physical and physiological differences between individuals, the management of nutritional inadequacy has to be tailored individually.
Micronutrient inadequacies would increase the risk of adverse health outcomes in older adults, such as immune function, frailty, osteoporosis, etc., through multiple pathways related to cell differentiation, oxidative stress, muscle and bone metabolism, inflammation, and decreased immunity23. As aforementioned, the micronutrient intake of many older adults is insufficient. Accordingly, MVM supplementation would facilitate older adults to meet their micronutrient requirements.
A randomised, double-blind, placebo-controlled study by Michels et al. (2023), which recruited 35 healthy men aged >67 years, indicated that MVM supplementation for at least 6 months improved blood concentrations of pyridoxal phosphate, calcifediol, α-tocopherol, and β-carotene concentrations. Remarkably, those in the placebo group showed declines in blood vitamin concentrations and an increased prevalence of suboptimal vitamin status during the study period (Figure 2). Moreover, MVM supplementation was reported to limit declines in cellular oxygen consumption rate in monocytes24. Based on the results, MVM supplementation is needed to ensure optimal vitamin status. It potentially plays a role in maintaining immune health in older adults.
Figure 2. Differences in the changes in blood micronutrient concentrations in participants with MVM supplementation against those with placebo24
In addition to increasing nutritional intake, high-quality clinical data showing the effectiveness of MVM supplementation in improving health outcomes in older adults are emerging. For instance, in the recent clinical study by Kim and Park (2023), which involved 2,478 people aged ≥65 years who participated in the Korea National Health and Nutrition Survey 2018–2020. The results revealed that the proportion of insufficient nutritional intake ranged from 6.2% to 80.5% for men and 21.2% to 82.4% for women, depending on the nutrients. Essentially, the results further showed that MVM supplementation (n=308) was associated with lower rates of inadequate nutritional intake compared to the food-only group (n=2,170, Figure 3A and 3B)25.
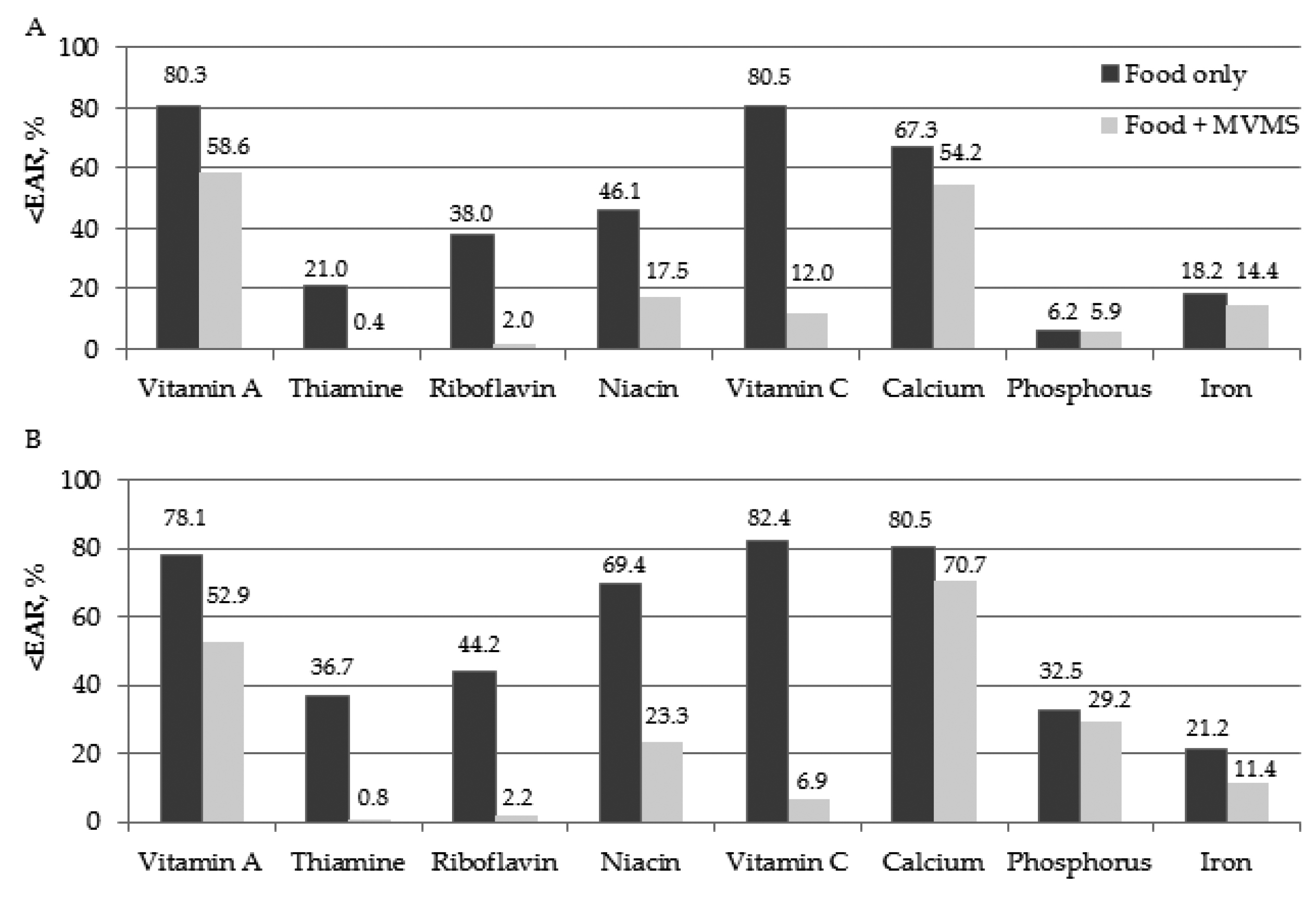
Figure.3 The percentage of older adults whose intake was below the estimated average requirement in (A) males and (B) females25, EAR: estimated average requirement, MVMS:MVM supplementation
On the other hand, the benefits of MVM supplementation in improving cognition in older adults were demonstrated in the COSMOS-Mind trial (2022), a randomised two-by-two factorial 3-year trial enrolling 2,262 participants. The results indicated that daily MVM supplementation (Centrum Silver, Haleon) resulted in a significant benefit on global cognition versus placebo (p=0.007, Figure 4). Although former epidemiological studies supported for the cognition-enhancing effects of flavonoids, cocoa extract, which contains high quantities of flavanols, yielded no significant effect on global cognition versus placebo (p=0.28). Notably, MVM supplementation also benefited memory and executive function26.
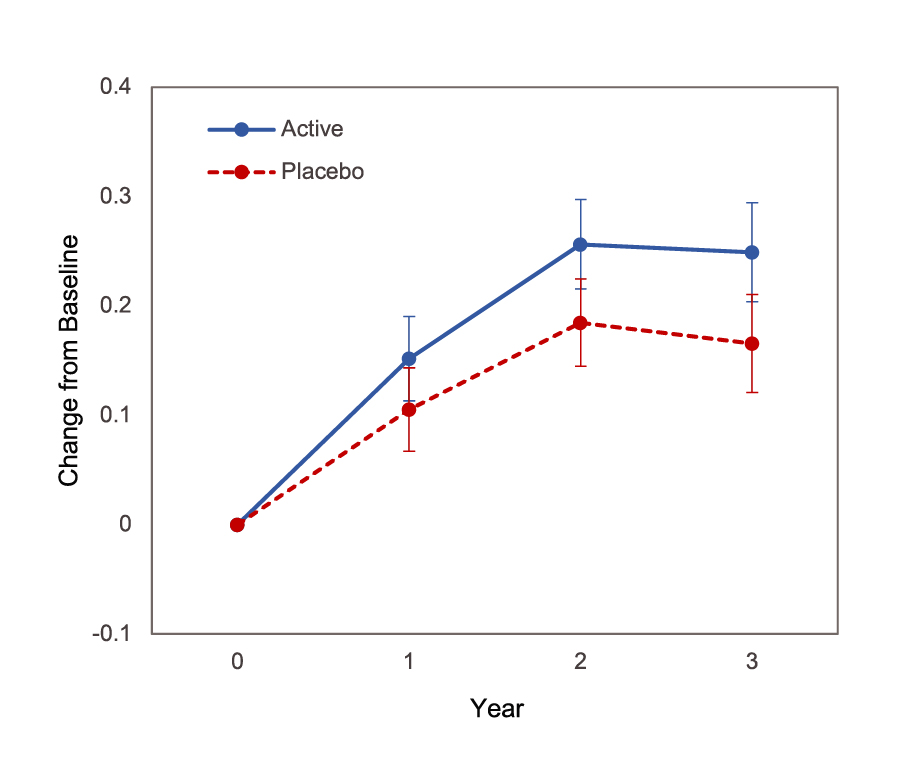
Figure 4. Three-year change in episodic memory composite by assignment to daily MVM supplementation26, Active: MVM supplementation
Interestingly, the results suggested that the MVM cognitive benefits may be more pronounced among older adults with cardiovascular diseases. Moreover, based on the difference in composite scores, 3 years of MVM supplementation appeared to have slowed ageing by 1.8 years, or by 60%26.
In the COSMOS-Web trial, an ancillary study of the COSMOS trial involving 3,562 older adults, daily MVM supplementation for 3 years resulted in a significantly better ModRey immediate recall test at 1 year (p=0.025), and across the 3 years of follow-up on average compared to placebo (p=0.011, Figure 5)27. More recently, the clinic sub-cohort of COSMOS trial (COSMOS-Clinic), which included 573 participants, indicated that daily MVM supplementation leads to a significantly more favourable 2-year change in episodic memory.
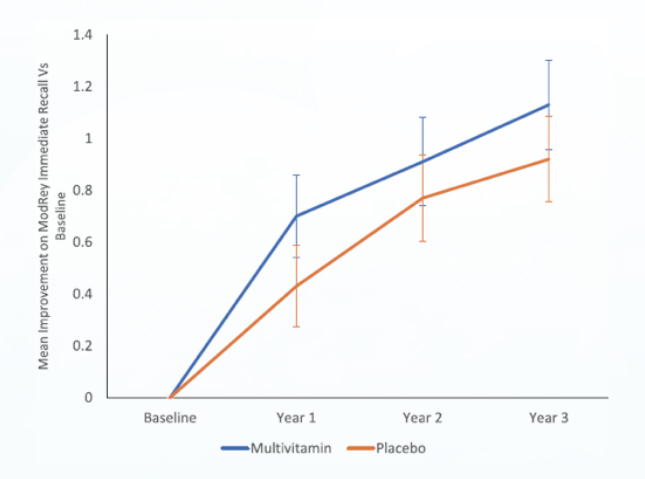
Figure 5. Mean improvement on ModRey immediate recall between treatment groups27, error bars: 95% CIs
Given the study design and the large sample sizes, the COSMOS trial and its ancillary studies provided high-quality evidence confirming the benefits of MVM supplementation on cognitive improvement in older adults. Notably, MVM supplementation holds promise as a safe and accessible approach to maintaining cognitive health27. Meta-analysis further supports that MVM supplementation reduces cognitive ageing by 2 years28. Of course, further investigations of the impacts of MVM supplementation on other organ systems is highly desirable. nonetheless, MVM supplementation should be avoided in patients with liver or kidney diseases and those who had organ transplants.
Polypharmacy is common among older adults, especially those with chronic diseases. Practically, roughly 70% of older adults aged >70 years take 2 or more medications daily, and many people take more than 3. Common medications prescribed to older patients include anti-hypercholesteraemic, anti-hypertensives, antacids, anti-coagulants, analgesics, proton pump inhibitors (PPIs), hypoglycaemics, and diuretics29.
Remarkably, many medications hinder micronutrient absorption. PPIs have been reported to impair the absorption of vitamin B12, vitamin C, and iron, whereas metformin would reduce the status of vitamin B12 and folate. Furthermore, diuretics are associated with disturbances in electrolyte homeostasis, including magnesium and zinc29. Thus, older adults taking multiple medications are at risk of micronutrient inadequacy.
To evaluate whether MVM supplementation would improve the nutritional status of older adults receiving medication treatments, a randomised control trial (RCT) was conducted by Chen et al. (2020). In the trial, 54 adults on ≥1 chronic drug therapy were randomly assigned to receive MVM supplementation or placebo for 16 weeks. The results indicated that MVM supplementation had a greater change in nutrient status after 16 weeks than the placebo group for serum folate (7.5 vs –1.6 ng/mL, p<0.0001), vitamin B12 (159.2 vs –33.9 pg/mL, p=0.007), and plasma vitamin C (0.2 vs 0.0 mg/dL, p=0.004). Based on the findings, MVM supplementation improved the levels of vitamins B12, C and folate in older adults receiving drug therapies29.
To optimise the nutritional status of older adults, the first step is to evaluate the amount of intake. Although measuring micronutrient levels is not a usual practice, it can be considered for potential cases of micronutrient inadequacy, such as those with low intake or symptoms developed. Essentially, under-supplementation is not good, but over-supplementation is unwanted neither. The measurement of micronutrient levels would guide MVM supplementation protocol, such as using more specific supplements.
While emerging clinical data advocate MVM supplementation in countering micronutrient inadequacy and improving the nutritional status of older adults, there is no consensus on the optimal level of micronutrients. Thus, a clear definition of the appropriate levels of micronutrients is desirable. In order to provide a comprehensive understanding on patients’ nutritional status, developing affordable clinical tests for measuring micronutrient levels is a key mission for the professionals in nutrition discipline.
By virtue of its effectiveness in ensuring micronutrient adequacy demonstrated in the clinical studies highlighted above, MVM supplementation potentially improves physical health and overall wellbeing for people of all ages, particularly the older populations. Given the long-term improvement in global cognition, episodic memory, and executive function in older adults has been reported, prospective works investigating the long-term outcomes of MVM supplementation on overall quality of life are highly desirable.
References
1. Ageing and health. https://www.who.int/news-room/fact-sheets/detail/ageing-and-health (accessed Nov 5, 2024). 2. Wallace et al. J Nutr Gerontol Geriatr 2019; 38: 307–28. 3. Tulchinsky. Public Health Rev 2010; 32: 243–55. 4. Park et al. J Nutr Elder 2008; 27: 297–317. 5. Watanabe et al. Eur J Nutr 2022; 61: 2451. 6. Kiani et al. J Prev Med Hyg 2022; 63: E93. 7. Food and Agriculture Organization of the United Nations, World Health Organization. Chapter 3. Human Vitamin and Mineral Requirements - Report of a joint FAO/WHO expert consultation 2001. 8. Food and Agriculture Organization of the United Nations, World Health Organization. Chapter 9. Human Vitamin and Mineral Requirements - Report of a joint FAO/WHO expert consultation 2001. 9. Food and Agriculture Organization of the United Nations, World Health Organization. Chapter 10. Human Vitamin and Mineral Requirements - Report of a joint FAO/WHO expert consultation 2001. 10. Baj et al. J Clin Med 2020; 9: 1901. 11. Food and Agriculture Organization of the United Nations, World Health Organization. Chapter 14. Human Vitamin and Mineral Requirements - Report of a joint FAO/WHO expert consultation 2001. 12. Avila et al. Met Ions Life Sci 2013; 13: 199. 13. Mustafa Khalid et al. Int J Environ Res Public Health 2022; 19: 15722. 14. Wylenzek et al. Arch Gynecol Obstet 2024; 310: 2235. 15. Houshialsadat et al. Eur J Nutr 2024; 63: 135–44. 16. Ter Borg et al. Br J Nutr 2015; 113: 1195. 17. Centre for Food Safety HKSAR. The First Hong Kong Total Diet Study: Minerals. 2014. 18. Brownie. Int J Nurs Pract 2006; 12: 110–8. 19. Baugreet et al. J Food Sci 2017; 82: 848–55. 20. Salazar et al. Gut Microbes 2017; 8: 82. 21. Jackson et al. Genome Med 2016; 8. DOI:10.1186/S13073-016-0262-7. 22. Jophlin et al. Curr Opin Gastroenterol 2024; 40: 112–7. 23. Inzitari et al. J Nutr Health Aging 2011; 15: 599–604. 24. Michels et al. Nutrients 2023; 15. DOI:10.3390/NU15122691. 25. Kim et al. Nutrients 2023; 15. DOI:10.3390/NU15071561. 26. Baker et al. Alzheimer’s & Dementia 2023; 19: 1308–19. 27. Yeung et al. Am J Clin Nutr 2023; 118: 273–82. 28. Vyas et al. Am J Clin Nutr 2024; 119: 692–701. 29. Chen et al. J Diet Suppl 2022; 19: 20–33.